KERATOCONUS
Keratoconus is a progressive condition of the cornea that results in distorted or blurred vision that is difficult to correct with standard glasses or contact lenses.
What is keratoconus?
Keratoconus is a disorder that causes progressive thinning and distortion of the cornea (the clear dome at the front of the eye). The cornea normally has a rounded shape but with keratoconus, the thinned area bulges forward to produce a cone-like distortion which reduces vision.
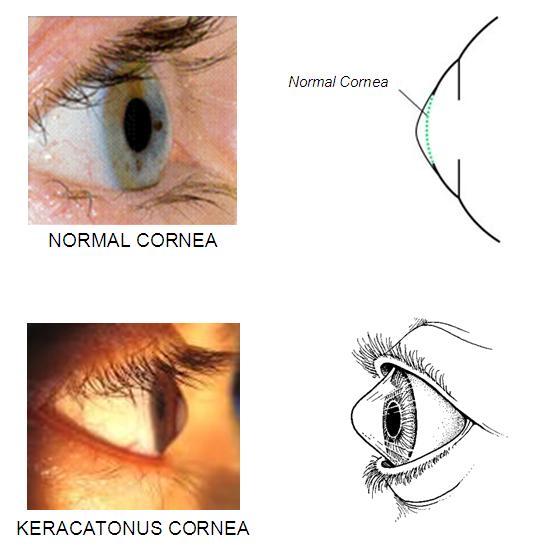
Example of a normal cornea compared to an eye with keratoconus.
Keratoconus affects people regardless of race or sex. Most patients develop keratoconus in their late teens to early twenties. Although it can begin at any age, the condition rarely develops after the age 30. It is a progressive disorder that may progress rapidly or sometimes take years to develop. It usually affects both eyes but often the disease develops asymmetrically.
What causes keratoconus?
The exact cause of keratoconus is unclear. Keratoconus is considered to be a genetic condition, as it is common to have a family member or relative with keratoconus. Many patients with keratoconus also have allergies, eczema and asthma but the link to allergic disease remains unclear.
Many patients who have the disorder report vigorous eye rubbing which should be avoided as it is thought to weaken the cornea.
How is it diagnosed?
Unfortunately it is not uncommon for keratoconus to be misdiagnosed. Changes in vision correction and measurement of corneal irregularity by an experienced practitioner can detect early keratoconus.
It is important to diagnose keratoconus early so treatment for progression can be initiated as soon as possible.
Treatment options
Contact lens fitting
Glasses or soft contact lenses often provide adequate vision for mild keratoconus. As the disorder progresses and the cornea becomes increasingly distorted, specially designed soft lenses often work well.
In more advanced keratoconus, rigid gas permeable (hard) contact lenses are usually the best choice for vision correction.
Customising and designing contact lenses for keratoconus is an intricate process. This requires a skilled and experienced practitioner to fine-tune the fit and prescription over a number of visits. In some cases, the process may take many months. The lenses will need to be refitted regularly to maintain good vision and lens comfort. A poorly fitting lens can cause scarring on the eye surface as well as discomfort and poor vision.
Barry & Sargent Optometrists use the sMap 3D topographer which obtains a detailed map of the cornea and front of the eye. These maps are much like a fingerprint in that no two are the same. We offer this advanced mapping technology to provide contact lenses that optimally fits the cornea and surface of the eye. This allows us to provide excellent vision and comfort.
Contact lens subsidy
NZ residents with keratoconus may be eligible for a Ministry of Health subsidy towards the fitting and supply of contact lenses. Although the subsidy generally does not cover all the associated costs, it will significantly bring down costs for the patient.
Corneal collagen cross-linking (CCXL)
Corneal collagen cross-linking (CCXL) is a procedure that can be performed to prevent progression of keratoconus. CCXL works by saturating the cornea with custom-made riboflavin drops, which are activated by UV light, to increase the collagen cross-links. These natural “anchors” within the cornea strengthen the cornea which can halt the weakening that is occuring.
CCXL is not a cure for keratoconus nor does it reverse any change that has already occurred. The aim of this treatment is to slow the progression of keratoconus and thereby prevent further deterioration in vision. Glasses or contact lenses will still be needed following the CCXL treatment, although a change in prescription may be required.
Corneal transplant
A corneal transplant may be indicated if keratoconus progresses and contact lens wear becomes unsuccessful or the cornea becomes scarred. Although there is some risk of tissue rejection, corneal transplants have a high rate of success.